When thinking of male body parts that bend, the penis probably isn’t one of the body parts that come to mind. Yet, for some men with Peyronie’s disease, having a curved penis or curved erection is a normal part of their sex life.
With the ability to make sex painful and difficult, penis curvature can impact a man’s mood, self-esteem, and personal relationships. So, while erectile dysfunction and premature ejaculation are reasonably well-known male sexual dysfunctions, Peyronie’s disease is still relatively unheard of.
So it’s time to shine a light on this rare sexual health condition affecting Aussie blokes.
What is Peyronie’s disease?
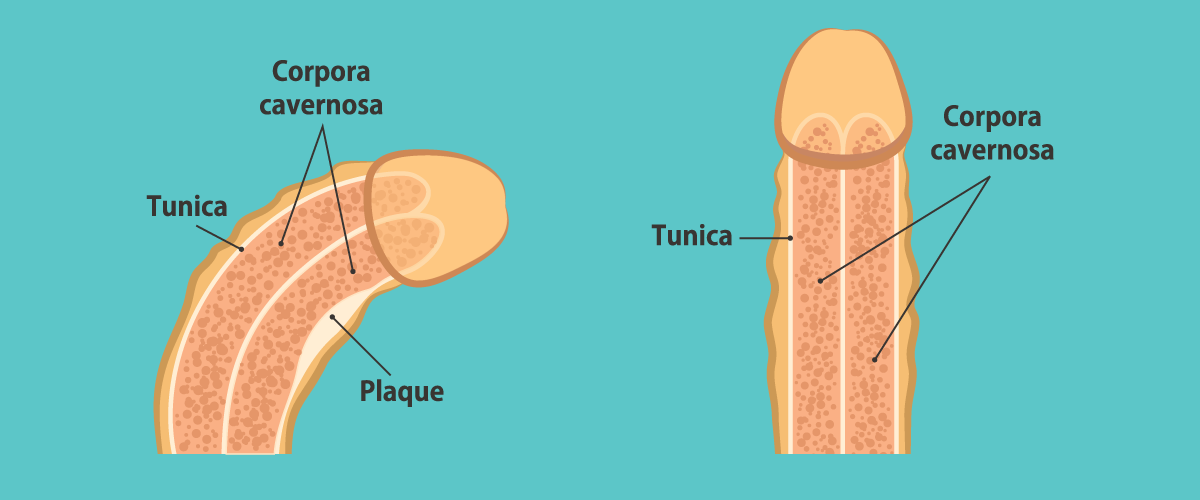
Peyronie’s disease is a disorder in which scar tissue, called plaque, builds up inside the thick elastic membrane of the penis called the tunica albuginea – the part of the penis responsible for keeping a penis firm during an erection. As it develops, the plaque pulls on the surrounding penile tissues, causing penile curvature during an erection.
Penis curves can cause painful erections and ejaculation problems and make sexual intercourse painful, difficult, and even impossible in many cases. Penile curvature can also have a psychological impact, causing low self-esteem, anxiety and depression (find out the difference between anxiety and depression). Peyronie’s disease is a relatively rare condition, and it is most often seen in middle-aged men.
The two phases of Peyronie’s disease
Peyronie’s disease occurs in two phases: the acute phase and the chronic phase.
The acute phase
The acute phase is when the plaque forms and can last up to 18 months. During the acute phase:
-
The penis starts to curve
-
Inflammation may occur
-
Penile pain may be experienced without an erect penis
-
Painful erection may result when scars develop
The chronic phase
The chronic phase of Peyronie’s disease is the period after plaque has formed, typically 12 to 18 months after the first symptoms appear. During the chronic phase:
-
Plaque buildup and penile curvature may stabilise without worsening
-
Penile pain may lessen
-
Erectile dysfunction may develop or worsen
Symptoms of Peyronie’s disease
Symptoms of Peyronie’s disease include:
-
Plaque buildup in the penis
-
Painful erections
-
Penile pain
-
Difficulty urinating
-
A lump on the penis
-
Curvature of the penis during erection
-
Sexual and urinary problems
If you suspect that you may have Peyronie’s disease, it is important to see a doctor who can diagnose Peyronie’s disease and prescribe an appropriate treatment plan.
What causes Peyronie’s disease?
The exact cause of Peyronie’s disease is unknown; however, it is thought to be the result of trauma to the penis. This could include injury during sex, masturbation, sport, or an accident.
Other possible theories suggest Peyronie’s disease may be caused by inflammation or infection of the tissues in the penis. It is also possible that Peyronie’s disease results from an autoimmune reaction, where the body mistakenly attacks the tissue of the penis. In some cases, Peyronie’s disease may be caused by a genetic mutation.
Peyronie’s disease is not contagious or caused by any known transmittable disease.
Why is it called Peyronie’s disease?
Peyronie’s disease is named after Francois de la Peyronie, a French surgeon who first described the condition in 1743. At the time, Peyronie was a personal physician to King Louis XIV of France, and his descriptions of the condition and its treatment were widely accepted and circulated among the medical community. As a result, the condition came to be known as Peyronie’s disease in his honour.
How common is Peyronie’s disease?
The exact prevalence of Peyronie’s disease is difficult to determine, but it is estimated to affect anywhere from 3-9% of men at some point in their lives¹⁻³. The condition is more commonly seen in older men, typically those over the age of 40.
It’s important to note that Peyronie’s disease may be underdiagnosed due to men’s reluctance to discuss their symptoms with their healthcare providers. Additionally, the prevalence of the condition may be increasing due to factors such as an aging population and improved survival rates for men with underlying medical conditions that can increase the risk for Peyronie’s disease.

Who is more likely to have Peyronie’s disease?
Certain people are at a higher risk of developing Peyronie’s disease, including those who:
-
Engage in rough and vigorous sexual activities that may cause micro-injuries to the penis
-
Engage in rough and vigorous non-sexual activities, such as sports, that may cause micro-injuries to the penis
-
Have a family history of Peyronie’s disease
-
Have diabetes
-
Have erectile dysfunction
-
Have a history of prostate cancer treatment with surgery
-
Have certain connective tissue disorders
-
Have certain autoimmune disorders
Risk factors of Peyronie’s disease
Risk factors that have been associated with Peyronie’s disease include:
Age
Peyronie’s disease is an inflammatory condition affecting the connective tissue of the penis, causing scar tissue formation. When scar tissue forms, it can lead to pain and difficulty achieving or maintaining an erection. Age is a risk factor for Peyronie’s disease because the connective tissue in the penis becomes less elastic with age. This makes it more susceptible to injury and inflammation. Peyronie’s disease is more common in middle-aged and older men but can occur at any age.
Family history
In some cases, family history may be a risk factor. Peyronie’s disease is more common in men who have a father or brother with the condition. It is not clear why family history may be a risk factor; it is believed that there may be a genetic component.
Smoking
Smoking is a risk factor for Peyronie’s disease because it can damage the blood vessels and cause inflammation. This can lead to the formation of plaque, which can then cause the penis to bend or curve. Smoking can also make symptoms of Peyronie’s disease worse.
Smoking and dealing with Peyronie’s disease? Find out how to quit vaping or smoking with clinically proven quit-smoking treatments online.
Trauma
Although the exact cause of Peyronie’s disease is unknown, it is believed to be the result of trauma to the penis. Trauma may include injury during sex, sports, or even rough handling during masturbation. It may also be the result of surgery that causes the formation of scar tissue in the penis.
Diabetes
One of the most common risk factors for Peyronie’s disease is diabetes. Diabetes can cause damage to the blood vessels and nerves in the penis, leading to the development of Peyronie’s disease. Diabetes is also a risk factor for other penile problems, such as erectile dysfunction. So, men with diabetes need to be aware of the risks and talk to their doctor if they develop any symptoms of Peyronie’s disease.
Connective tissue disorders
Certain connective tissue disorders, such as Dupuytren’s contracture (a condition that causes the fingers to bend) and Ehlers-Danlos syndrome, are risk factors for Peyronie’s disease because they can weaken the tissues that support the penis. This can cause the penis to bend or curve, which can lead to Peyronie’s disease. If you have a connective tissue disorder, it is important to talk to your doctor about the risks of Peyronie’s disease.
How does Peyronie’s disease affect your sex life?
As a men’s sexual health condition that causes the penis to curve or bend, Peyronie’s disease can cause pain and difficulty with erections. In some cases, it can also lead to erectile dysfunction and significantly impact your sex life, both physically and emotionally.
If you are experiencing pain during sex or cannot have an erection, it can be challenging to enjoy intimacy with your partner. Peyronie’s disease can also cause anxiety and low self-esteem, further affecting your sexual relationship. If you are concerned about how Peyronie’s disease impacts your sex life, talk to your doctor or a sex therapist. They can provide information and resources to help you manage the condition and improve your sexual relationships.

Peyronie’s disease and erectile dysfunction (ED)
Erectile dysfunction is the inability to get or keep an erection firm enough for sexual intercourse. It can happen at any age but is more common in men over 40. Erectile dysfunction can be caused by psychological or physical factors or a combination of the two. Psychological causes include stress, anxiety, and depression. Physical causes include conditions like diabetes, heart disease, obesity, and Peyronie’s disease.
Learn more about the causes of erectile dysfunction.
When a man has Peyronie’s disease, the buildup of plaque in the penis that causes penile curvature can cause pain and difficulty when trying to form an erect penis, and erectile dysfunction can result.
There is a possibility that erectile dysfunction (ED) treatments may help to improve the symptoms of erectile dysfunction caused by Peyronie’s disease. Therapies such as penile injections or penile traction devices may help to straighten the penis and improve erections, and surgery may also be an option. However, it is important to speak to a doctor before starting any treatment for erectile dysfunction and Peyronie’s disease.
Peyronie’s disease and depression
Peyronie’s disease can significantly impact a man’s quality of life, and it has been linked to depression, with roughly half of all Peyronie’s sufferers having depression⁴. As a rare connective tissue disorder that causes pain and difficulty forming an erection, Peyronie’s disease can lead to feelings of insecurity, anxiety, and depression.
If you’re dealing with depression due to Peyronie’s disease, it’s important to seek treatment. Talk to your doctor about your options, which may include medication, therapy, or surgery. Peyronie’s disease can be a complex condition to deal with, but with the right treatment, it is possible to manage the symptoms and live a relatively normal life.
Treating Peyronie’s disease
The treatment of Peyronie’s disease varies depending on the severity of the condition and the individual patient’s goals and preferences. In some cases, Peyronie’s disease may resolve on its own without any intervention, while in other cases, more aggressive treatment may be necessary.
Here are some common treatments to consider if you develop Peyronie’s disease:
- Observation: If the curvature of the penis is not significant and is not causing any pain or other symptoms, observation may be a reasonable approach. In some cases, the plaques that cause Peyronie’s disease may eventually shrink or disappear on their own.
- Medications: Nonsteroidal anti-inflammatory drugs (NSAIDs) or collagenase inhibitors may be used to reduce inflammation and soften the plaques that cause Peyronie’s disease.
- Penile traction therapy: This involves using a device that applies gentle tension to the penis to help straighten the curvature. Penile traction therapy has been shown to be effective in some cases, but its efficacy has been disputed by some experts.
- Surgery: If other treatments are not effective, surgical intervention may be necessary. There are several surgical options available, including plication surgery (where the curved side of the penis is stitched to itself to reduce the curvature) and penile prosthesis implantation.
It’s important to note that the decision to treat Peyronie’s disease should be made in consultation with a healthcare provider, who can help determine the best course of action based on the individual patient’s medical history and the severity of their condition.
Get your sexual health sorted!
Whether you’re having trouble staying erect or delaying ejaculation, stay on top of your sexual health with Stagger.
Sources
- “The Prevalence of Peyronie’s Disease: Results of a Survey of the French-Speaking Society of Andrology.” British Journal of Urology International, vol. 91, no. 7, 2003, pp. 751-753.
- “Prevalence of Peyronie’s Disease in Men Attending a Sexual Medicine Clinic.” Journal of Sexual Medicine, vol. 7, no. 3, 2010, pp. 1088-1093.
- “Prevalence of Peyronie’s Disease in Men Undergoing Urologic Evaluation.” Journal of Urology, vol. 185, no. 4, 2011, pp. 1228-1232.
- Levine, Laurence A. “The clinical and psychosocial impact of Peyronie’s disease.” The American journal of managed care vol. 19,4 Suppl (2013): S55-61
